Epidermolytic ichthyosis (old fashioned name "bullous congenital ichthyosiform erythroderma of Brocq")
This is a rare Mendelian keratinization disorder that is mostly inherited as an autosomal dominant trait. In a few families inheritance is autosomal recessive. Occasionally, the disease becomes manifest in a form of a nevus often affecting only a small part of the skin surface. However, there is the possibility that in the next generation a full blown disease affecting the entire skin occurs.
The disease is characterized by erythema, scaling and blistering. At birth there is usually a generalized erythema (medical term: erythroderma) and parts of the upper most skin layers peel off. This can look more “horrible” and more “dangerous” than is really the case. The peeling off of the skin is rather superficial and mostly improves after a few days. Of course, like other neonates suffering from congenital ichthyosis, admittance to a neonatal intensive care unit immediately after birth is necessary.
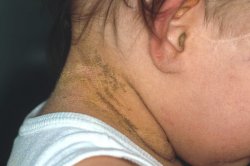
Indeed, there is true blister formation in the skin. Because of the superficial localization the roof of the blister is easily destroyed so that often it is not possible to note intact blisters. A few patients have only for a few days increased blistering, while in others this increase blistering continues for several years. With increasing age the proneness for blistering decreases. It is replaced by a stronger keratinization (cornification). The scaling looks different from most types of ARCI or from lamellar ichthyosis since not so much scales, but keratinized cones predominate resulting in a wart-like clinical picture. The keratoses are more pronounced in the major body folds.
The histologic architecture is quite disturbed and results in a pathognomic histopathology allowing a rapid diagnosis by a skin biopsy taken immediately after birth. The basic defect concerns either keratin 1 (mostly with clinical involvement of palms and soles) or keratin 10 (usually without involvement of palms and soles). Keratins are responsible for the assembly of cell filaments (tonofilaments) providing the keratinocytes stability and adherence. If there is a genetic mutation in e.g. keratin 10, molecular superstructures like the tonofilaments are assembled in the wrong way resulting in a loss of function of these superstructures. This means that keratinocytes lose their normal adherence and a blister is formed. The enormously increased keratinization seen in the disease must be viewed as a repair process with the aim of compensating the defect of the epidermal barrier function.
